Alisson Lima Andrade; Luiz Vieira Sá II
DOI: 10.17545/eOftalmo/2024.0017
ABSTRACT
Posterior lenticonus is a rare eye anomaly in children that affects the lens growth and may lead to amblyopia and strabismus. Although its cause remains unknown, numerous hypotheses have been proposed. Herein, we have reported the case of a 3-year-old female without syndromic findings or a family and ophthalmological history. A white reflex was observed in her left eye. Other ophthalmologic examinations did not reveal any other malformations or diseases. Lensectomy and intraocular lens placement was performed to prevent the development of amblyopia. A satisfactory postoperative outcome was achieved in the child.
Keywords: Posterior lenticonus; Cataract; Cataract extractions; Lens opacity.
RESUMO
O lenticone posterior é uma anomalia ocular rara que afeta o desenvolvimento do cristalino, podendo levar à ambliopia e estrabismo em crianças. Sua causa permanece desconhecida, entretanto diversas hipóteses têm sido estudadas. Reportamos um relato de caso de uma menina de 3 anos de idade sem achados sindrômicos, histórico ocular ou familiar. Ela desenvolveu reflexo opaco no olho esquerdo e o exame oftalmológico subsequente não evidenciou qualquer outra malformação. Foi submetida à lensectomia e implante de lente intraocular como prevenção contra ambliopia, sendo alcançado resultado pós-operatório satisfatório.
Palavras-chave: Cápsula posterior do cristalino; Catarata; Extração de catarata; Opacidade do cristalino.
INTRODUCTION
Posterior lenticonus is a rare lens anomaly without a known etiology, with a prevalence of 1-4 in 100,000 children. It was first described by Fritz Meyer in 18881. Ophthalmologic examination reveals a conical-shaped protrusion in the posterior capsule of the lens toward to the vitreous. This is classically described as an "oil droplet", and it is usually associated with lens opacity2.
Several theories have been proposed regarding the origin of a posterior lenticonus, including posterior capsule traction by hyaloid artery remnants, epithelial cell growth within the posterior capsule, and inherited posterior capsule weakness3. Makley Jr histologically examined eyes with a posterior lenticonus and identified epithelial cells, organized as a monolayer, under the capsule at the lenticonus site. However, another group of cells, organized as multiple layers, was observed over the apex. Their cell structure was similar to that of lens fibers4.
Posterior lenticonus progression may lead to refractive disorders, causing visual acuity reduction and amblyopia in children. Thus, surgical treatment is often required to avoid permanent visual loss.
CASE REPORT
A mother visited our university eye care center with her 3-year-old daughter in whom she had noticed a left eye opacity in the last 2 months. She denied any gestational or perinatal diseases.
An eye examination under general anesthesia revealed a corneal diameter of 12.5 mm in both eyes and a lens thickness of 3.75 mm and 4.04 mm in the right eye (OD) and left eye (OS), respectively. The axial length was 21.11 mm and 21.16 mm in the OD and OS, respectively. The corneal curvature was 44.00 a 178° x 45.37 a 88° in the OD and 43.37 a 170° x 45.50 a 80° in the OS. Anterior biomicroscopy revealed a normal lens in the OD and a posterior lenticonus in the OS. Central opacification of the lens was observed in the OS, without any abnormalities on fundoscopic examination. Ocular ultrasound revealed a bulge in the posterior capsule of the OS lens, which was suggestive of a posterior lenticonus (Figure 1).
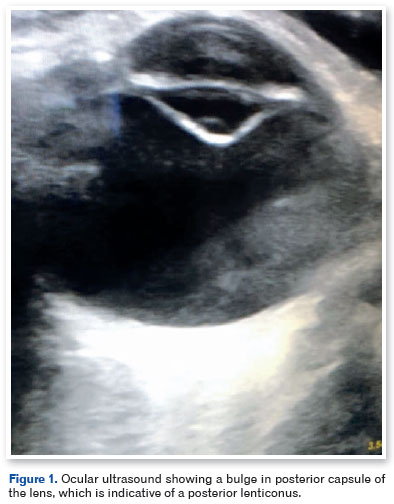
Anterior vitrectomy, lensectomy, posterior capsulotomy, and intraocular lens (IOL) insertion (+21.5 D), with a final target refraction of +5.00 D), were performed in the OS. Postoperatively, optical correction (bifocal glasses) was prescribed for the OS in addition to an eye patch for the OD.
Over a 3-year follow-up period, the patient and her mother have reported no complaints. The patient has adapted well to the glasses, and the corrected visual acuity is 20/20 in the OD and 20/30 in the OS. At the last follow-up, the ophthalmological examination revealed a correctly positioned IOL without any abnormal findings.
DISCUSSION
Posterior lenticonus develops sporadically and unilaterally (more commonly) or bilaterally. It occurs more frequently than anterior lenticonus and is sometimes associated with cataracts5. Some studies have demonstrated an X-linked genetic inheritance in some patients with unilateral and non-syndromic disease, in addition to a autosomal dominant transmission with variable expression6.
Vivian et al. reported that a bilateral presentation of posterior lenticonus has a greater association with genetic inheritance than the unilateral form7. Posterior lenticonus is rarely associated with other malformations such as microcornea, microphthalmos, uveal colobomas, and persistent fetal vasculature. Furthermore, it is often associated with Alport's syndrome, an X-linked disorder that presents with progressive nephritis, which can lead to renal failure, sensorineural hearing loss, and ophthalmic changes. Halawani et al. reported the case of a patient with Alport's syndrome and bilateral anterior lenticonus who developed posterior lenticonus 8 years after the initial diagnosis5,8.
Our patient presented with unilateral posterior lenticonus and no family history of eye diseases, ocular malformations, or systemic diseases. It appeared to be a sporadic case that was not related to an X-linked or autosomal dominant inheritance.
We performed a lensectomy and IOL insertion because of the high probability of lenticonus progression that is associated with lens opacity. This would have led to a large refractive defect, significantly reducing the visual acuity of the child. This approach aids in avoiding amblyopia and strabismus. Chen et al. reported that children with a posterior polar cataract (≤3 mm) and posterior lenticonus who underwent lensectomy had a better final visual acuity than those who were conservatively managed2,9.
REFERENCES
1. Reese WS. Posterior Lenticonus. Trans Am Ophthalmol Soc. 1928;26:339-45.
2. Cheng KP, Hiles DA, Biglan AW, Pettapiece MC. Management of posterior lenticonus. J Pediatr Ophthalmol Strabismus. 1991;28(3):143-9; discussion 150.
3. Khalil M, Saheb N. Posterior lenticonus. Ophthalmology. 1984;91(11):1429-30, 43A.
4. Makley Jr. TA. Posterior lenticonus; report of a case with histologic findings. Am J Ophthalmol. 1955;39(3):308-12.
5. Halawani LM, Abdulaal MF, Alotaibi HA, Alsaati AF, Dakhil TAB. Development of Posterior Lenticonus Following the Diagnosis of Isolated Anterior Lenticonus in Alport Syndrome. Cureus. 2021;13(1):e12970.
6. Russell-Eggitt IM. Non-syndromic posterior lenticonus a cause of childhood cataract: evidence for X-linked inheritance. Eye (Lond). 2000;14(Pt 6):861-3.
7. Vivian AJ, Lloyd C, Russell-Eggitt I, Taylor D. Familial posterior lenticonus. Eye (Lond). 1995;9(Pt 1):119-23.
8. Khokhar S, Dhull C, Mahalingam K, Agarwal P. Posterior lenticonus with persistent fetal vasculature. Indian J Ophthalmol. 2018;66(9):1335-1336.
9. Chen H, Chen W, Wu XH, Lin ZL, Chen JJ, Li XY, et al. Visual outcomes of surgical and conservative treatment in children with small posterior polar cataracts and posterior lenticonus. Int J Ophthalmol. 2021;14(1):64-71.
AUTHORS INFORMATIONS |
|
 |
» Alisson Lima Andrade https://orcid.org/0000-0001-6067-1656 https://lattes.cnpq.br/4884165924641981 |
 |
» Luiz Vieira Sá II https://orcid.org/0000-0002-4164-8714 https://lattes.cnpq.br/6324350500089081 |
Funding: No specific financial support was available for this study.
Conflict of interest: None of the authors have any potential conflict of interest to disclose.
Received on:
March 27, 2023.
Accepted on:
June 14, 2024.